It is too easy to go about our busy lives and not notice physical or mental illness symptoms. Our body has built-in warning systems which alert us to the signs of mental illness that we need to pay attention to.
Here are five warning signs of mental illness to watch for, especially when you have two or more of these symptoms.
- Long-lasting sadness or irritability
- Extremely high and low moods
- Excessive fear, worry, or anxiety
- Social withdrawal
- Dramatic changes in eating or sleeping habits
Below are a couple of self-report tests for warning signs of mental illness, which you can complete and score to see if you might be experiencing clinical depression. Keep in mind that depression can include anxiety symptoms, and when combined with an extreme shift in moods, then bipolar disorder is further evaluated. There are many other self-report mental health screening tools that you may consider, i.e., PBHCI – Mental Health Screening.
The PHQ-2 in Figure 1 Warning Signs of Mental Illness, below inquiries about the frequency of depressed mood and anhedonia over the past two weeks.
The PHQ-2 includes the first two items of the PHQ-9. The purpose of the PHQ-2 is not to establish a final diagnosis or to monitor depression severity, but rather to screen for depression in a “first step” approach. Patients who screen positive should be further evaluated with the PHQ-9 to determine whether they meet the criteria for a depressive disorder. When scoring the PHQ-2, the range is from 0-6.
The authors identified a PHQ-2 cutoff score of three.
1 is the optimal cut point for screening purposes and stated that a cut point of two would enhance sensitivity. Whereas a cut point of four would improve specificity.
Figure 1 Warning Signs of Mental Illness
The Patient Health Questionnaire-2 (PHQ-2)
(Kroenke, K. et al., 2003)
If you scored 3 or above, you might proceed to answer the questions in the self-report PHQ-9. The PHQ-9 in Figure 2 below is a multipurpose instrument for screening, diagnosing, monitoring, and measuring the severity of depression.
The PHQ-9 incorporates DSM-IV depression diagnostic criteria with other leading major depressive symptoms into a brief self-report tool. The tool rates the frequency of the signs that factors into the scoring severity index. Question 9 on the PHQ-9 screens for the presence and duration of suicide ideation.
In a follow-up, the non-scored question on the PHQ-9 screens and assigns weight to the degree to which depressive problems have affected the patient’s level of functioning. This tool is brief and useful in clinical practice.
The PHQ-9 can also be administered more than one time as an assessment tool to monitor improvement or increased levels of depression in response to treatment.
The PHQ-9 can make a tentative depression diagnosis. However, physical/environmental causes of depression, i.e., normal bereavement, or a history of manic/hypomanic episodes should be considered.
It is always best to ask your primary care provider if it would be helpful to be further evaluated by a mental health professional who can assist with psychotropic medication management and ascertain your levels of depression in response to the treatment plan.
Figure 2 Warning Signs of Mental Illness
The Patient Health Questionnaire-9 (PHQ-9)
(Kroenke, K. et al., 2001)
The overview for scoring the PHQ-9 is as follows:
Step 1: Questions 1 and 2 – Need one or both of the first two questions endorsed as a “2” or a “3” (2 = “More than half the days” or 3 = “Nearly every day”).
Step 2: Questions 1 through 9 – Need a total of five or more boxes endorsed within the shaded area of the form to arrive at the total symptom count (Questions 1-8 must be endorsed as a “2” or a “3,” and Question 9 must be endorsed as “1” a “2” or a “3”).
The use of the PQH-9 for treatment selection and monitoring is as follows:
Step 1: A depression diagnosis that warrants treatment or a treatment change, needs at least one of the first two questions endorsed as positive (“more than half the days” or “nearly every day”) in the past two weeks. Also, the tenth question, about difficulty at work or home or getting along with others should be answered with at least “somewhat difficult.”
Step 2: Add the total points for each of the columns 2-4 separately (Column 1 = several days; Column 2 = More than half the days, Column 3 = Nearly every day. Add the totals for each of the three columns together. This is the Total Score that equals the Severity Score.
Step 3: Review the Severity Score using the following TABLE for PHQ-9 Scoring:
++ If symptoms present > one month or severe functional impairment, consider active treatment.* If symptoms present > two years, then probable chronic depression which warrants antidepressants and psychotherapy (ask yourself, “in the past two years have I felt depressed or sad most days, even if I felt okay sometimes?”)
According to the National Alliance on Mental Illness (NAMI) each illness has its own set of symptoms, some combined, but here are some other common warning signs of mental illness in adults and adolescents.
- Confused thinking or problems concentrating and learning
- Extreme mood changes, including uncontrollable “highs” or feelings of euphoria
- Prolonged or strong feelings of irritability or anger
- Difficulties understanding or relating to other people
- Changes in sex drive
- Difficulty perceiving reality (delusions or hallucinations, in which a person experiences and senses things that don’t exist in objective reality)
- Inability to perceive changes in one’s own feelings, behavior, or personality (” lack of insight” or anosognosia)
- Abuse of substances like alcohol or drugs
- Multiple physical ailments without obvious causes (such as headaches, stomach aches, vague and ongoing “aches and pains”)
- Thinking about suicide
- Inability to carry out daily activities or handle daily problems and stress
- Intense fear of weight gain or concern with appearance
The good news is that you can go to your primary care provider and be prepared to talk about any of the symptoms you have been experiencing. Most primary care offices use the PHQ-2 and PHQ-9 as valid screening tools.
If you decide to complete the self-report brief screening tools, you may complete them and take them with you to your medical doctor. Some primary care physicians will feel comfortable prescribing an anti-depressant. Some of the primary care clinics like the Federally Qualified Healthcare Clinics (FQHC’s) offer same-day service with the medical provider and a behavioral health consultant, psychologist, or licensed mental health therapist. They form what is called a primary care team who works to promote healing for the “whole person.”
Most Common Mental Illnesses
Depression
Depression is a mood disorder. A person living with depression often experiences completely different thoughts before and after a depressive episode. This can be a result of a chemical imbalance in the brain and can lead to the person not understanding the options available to help them relieve their suffering. Many people who suffer from depression report feeling as though they’ve lost the ability to imagine a happy future, or remember a happy past. Often they don’t realize they’re suffering from a treatable illness, and seeking help may not even enter their mind. Emotions and even physical pain can become unbearable. They don’t want to die, but it’s the only way they feel their pain will end. It is a truly irrational choice. Suffering from depression is involuntary, just like cancer or diabetes, but it is a treatable illness that can be managed.
Bipolar Disorder
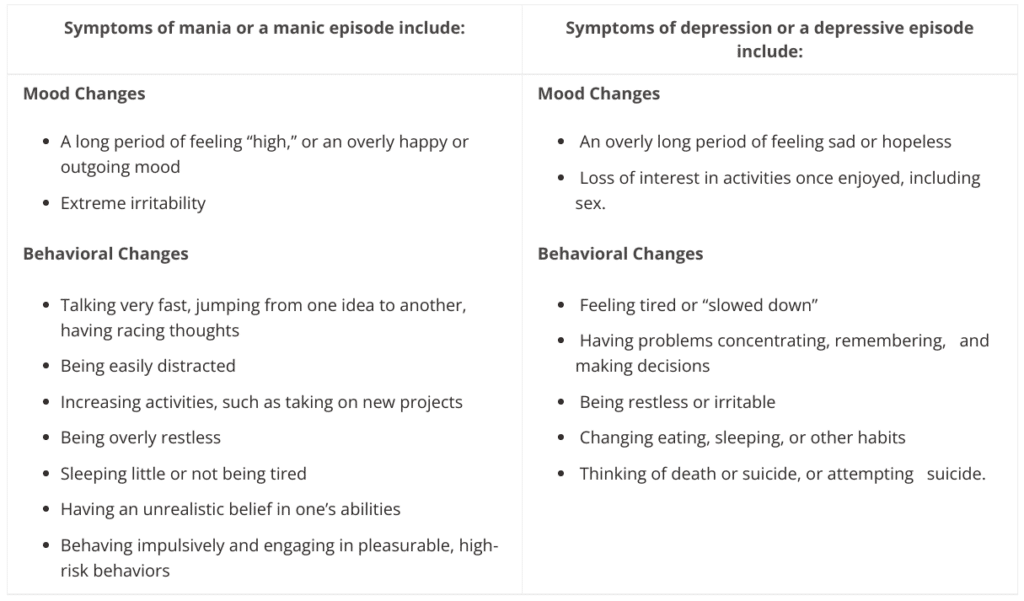
People with bipolar disorder experience unusually intense emotional states that occur in distinct periods called “mood episodes.” Each mood episode represents a drastic change from a person’s usual mood and behavior. An overly joyful or overexcited state is called a manic episode, and an extremely sad or hopeless state is called a depressive episode. Sometimes, a mood episode includes symptoms of both mania and depression. This is called a mixed state. People with bipolar disorder also may be explosive and irritable during a mood episode.
Extreme changes in energy, activity, sleep, and behavior go along with these changes in mood. Symptoms of bipolar disorder are described below. (“Bipolar Disorder and Suicidal Ideation – SAVE”)
(“Bipolar Disorder and Suicidal Ideation – SAVE”)
Borderline personality disorder
Because some people with severe BPD have brief psychotic episodes, experts originally thought of this illness as atypical, or borderline, versions of other mental disorders. While mental health experts now generally agree that the name “borderline personality disorder” is misleading, a more accurate term does not exist yet.
Most people who have BPD suffer from:
- Problems with regulating emotions and thoughts
- Impulsive and reckless behavior
- Unstable relationships with other people
Seeking Treatment
The first step is getting a diagnosis and learning about your choices for treatment. Treatment goals have objectives that can help improve your daily living activities (DLA’s) for functioning at work, home, church, and other activities. There is no “one size fits all types of treatment.” Treatment options may include psychotropic medication, counseling (therapy), social support and psycho-education.
Additionally, another first step is to love yourself and the significant others in your life enough to “lovingly accept help.” Affirm this – “For good and for bad, in sickness and in health, I love myself and others unconditionally.” When we do this, we can change, grow, and expand our life to reach out and offer help to others. When we are healthy, we feel better about ourselves and mindful of our blessings with deep gratitude for life.
Step 2 is to gain hope for healing to have clarity for knowing your life purpose. With faith in a “Higher Power,” you find meaning and purpose and grow stronger daily. Good Health is a blessing and we must be aware of any warning signs, so we can get help and begin to feel better. We must acknowledge self-care and know that “we are worth it.”
In Conclusion
To learn more about warning signs of mental illness click here, “The Tragedy of the Stigma of Mental Illness” and learn more about our WORTH program info@newroadstreatment.com.
Please stop by and see us. Our team would love to meet you! Find us here.
New Roads Behavioral Health 888-358-8998





